Nasal Turbinate – Concha
Nasal Cavity
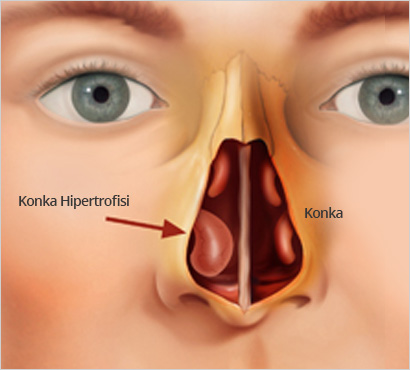
Turbinate/Conca is the medical term given to the long, narrow and curled bone shelf (similar in shape to an elongated sea-shell) that is located in the breathing passage of the nose. It is also referred to by other names in different languages – Turbine (Turbinate), Cornet being a few.
Before describing the formation of the Turbinate/Conca it will be best to describe the structure of the nasal area. The nose consists of two parallel tunnels, which are separated by a wall. If we were to slice cut cross-sections, from the beginning of the area, we will find a triangular shaped structure that gets bigger in size towards the middle part of the nose and then gets smaller again towards the rear part of the nose. From the middle part of these tunnels throughout the outer (lateral) wall is a long protrusion that extends along the nasal cavity and is known as the Turbinate.
Turbinate protrusions: Inferior - Middle – Superior - Superior Upper
The Turbinate shape is formed in a way that from the base to the top they shrink in size. They are similar to groove-like air passages that allow for inhaled air to flow steadily whilst acclimatizing the air inhaled. Most people will have three Turbinate though sometimes we do come across four. According to their position in the nasal passage they are given names. The largest one is located at the bottom is called ‘The Inferior Turbinate'; the one above this is called the ‘Middle Turbinate’ then the one on top of the middle turbinate is called the ‘Superior Turbinate’ and if another one is found to exist this is referred to as the ‘Superior Upper Turbinate’. There is a vast difference is size between the Inferior Turbinate in comparison to the other turbinate. Besides the difference in size there is one other factor that is a character of the Inferior Turbinate is that it is able to change it’s size. Due to this ability the Inferior Turbinate can assume the air filtration regulatory functions effectively.
The Middle Turbinate and Superior Turbinate are not known to have the ability to change in size. Their fixed structures provide the perfect environment for heat and moisture control of the air-inhaled. They also provide the function of directing the airflow and partly contribute to the ability to aroma/smell scents distinction as they hold scent-carrying cells.
The Inferior Turbinate is also referred to as the main organ of the nose this is due to its size, spanning from the entrance of the nose to the back exit; its ability to change its size thus the volume of airflow is controlled. In order to understand the full capability of this main organ I will need to further explain its full functions.
Inferior Turbinate
In the nasal cavity (vestibule – entrance of the nose area) directly behind the tunnel flaps is where the Inferior Turbinate starts and it is also the part where the air supply is taken in. The inferior turbinate is a leaf like layer of bone that extends into the nasal cavity from the sidewall of the nose. It is intertwined and wrapped with a multitude of blood vessels that are kept moist by a covering of mucosa. These blood vessels can adjust accordingly to specific changes by increasing and decreasing the amount of blood levels they can hold. The circumferential surface of the inferior turbinate can adapt due to its flexible structure; thus the inferior turbinate can at be in either inflated (swollen up) or deflated state like a balloon. Besides these functions these highly sensitive surfaces are also adept at performing other functions.
The type of mucosal tissue/membrane that covers the circumferential surface of the inferior turbinate is similar to the mucosal tissue that covers the surface of the entire nasal cavity except for the cells that are used in the function of sensing smell/aroma which are called the olfactory receptor cells. This surface tissue of mucosal membrane not only to acts as a protective covering surface for the formations underneath it; it also the ability to secrete a fluid from microscopic fountain like structures together with similar sized hair follicles that aid in sweeping fluids towards the back of the nasal area and the throat.
Nasal function and the role of the Inferior Turbinate
When we breath in air from our nose, if the air is cold, dry, warm or contaminated with tiny (microscopic) particles, before the air moves to the back of the throat, the air will go through a process of sensors that are able to perceive what has been inhaled and then decides either to warm, moisten and/or filter the air. Simultaneously all that has been sensed by the sensors are sent as signals to the brain, which then sends commands reflexively to the lungs to be prepared for the appropriate air intake – it will also recognize scents/aromas and thus direct and inform the appropriate zones.
The size/volume of the Inferior Turbinate changes its functioning ability in accordance with weather conditions, how the head is positioned (lying flat, standing etc), physical activity status (running, sleeping, exercising, flying etc) and even to psychological condition. As an example of the inferior turbinate nasal functioning it will build resistance in cold weather by inflating its size in volume with fluid inside the blood vessels. This is achieved by increasing its resistance to the air inhaled by increasing the mucosal secretions. This is the reason we have runny noses in cold weather.
All this work is amazingly orchestrated with such fine-tuning that a perfect balance is harmoniously achieved…
An understanding of the micro world is a necessity to perceive and appreciate the balance achieved by the fine functioning of the nose. Scientist and researchers specializing in the development of medical science use these types of information obtained so that they may continue finding solutions to diseases related to the nasal area thus hopefully benefit mankind.
Problematic Inferior Turbinate
The most common problem in medical practice for the Inferior Turbinate is an extreme resistance to air, i.e. cases where air is prevented from entering the nose. Basically put this is when the nasal area is congested it becomes problematic.
When this becomes problematic is when the nose is congested for more than just a couple of hours a day. These can be months and even years of blockages. Night congestions that interrupt sleep periods overnight. Congestions that mean you have to breath through your mouth…
One of the causes of congestion or the underlying cause may be an uncontrolled or inappropriate largeness/growth of the Inferior Turbinate. When a patient comes to a doctor with these complaints, that they can not breathe through their nose, the doctor will examine, recognize and evaluate the situation so that they can advise which course of action is most appropriate for the patient’s distress to be relieved.
Seeing that the most common problem with the Inferior Turbinate is the uncontrolled swelling, it would not be out of place to state that this same issue is one that is at the top of ENT physicians to find a remedy.
Surgical treatment of enlarged Inferior Turbinate
If after months or years of treatment, with specific measures taken and drug use with only short-term relief then these are cases that can only be corrected by surgery. The surgery is one of the smallest of operations performed in the nose, but still includes an intranasal intrusion; the Turkish Medical Association Alliance for minimum wage rates these operation costs very lowly.
However the price rating is accorded it is non-the-less a very highly skilled surgery that requires competence and expertise on the subject. The operations can be performed with the aid of a very fine piece of surveillance equipment used in medical operations called an Endoscope or open surgery using a surgical forehead lamp for visual aid during the operation. The patient will be guided by the physician in coming to a decision as to which will be the best way to undertake the operation, either with the use of general or local anesthesia.
There are several factors that are considered when planning the surgery. If possible any further damage to the turbinate is preferably avoided so as not to completely destroy the structure. Ideally the surgery is aimed to reduce the size of the turbinate. Then, an approach that protects the unique structure of the turbinate surface will largely selected. And, of course every measure will be taken to avoid any adverse affects of the operation as much as possible including the time off from work.
Commonly practiced techniques are as follows:
- Reducing the turbinate size using the heat effect, i.e. etching (cauterization or laser)
- The use of low radiofrequency devices to reduce the size using even lower heat treatment
- The use of a Microdebrider for the reduction of internal soft tissue of the turbinate
- Reducing the bone size of the turbinate or breaking the turbinate bone and turning then pushing it sideways
- Removing all or a portion of the turbinate
Whatever the technique chosen, it will mean eventually mean once the nasal respiratory resistance is normalized thus breathing will become a lot easier.
Risks of Turbinate surgery
As with any surgery there are risks of course of turbinate surgery too. However, I must state that comparatively they carry a very low risk in surgery.
The most common types of he risks seen are in the main as follows;
- Bone infections-prolonged wound healing
- Intra-nasal dryness, crusting
- Intranasal adhesions
- Bleeding
Last but not least ...
As operative doctors, we make great efforts and take all the measures we can to prevent risks from happening.
Success rates are extremely high, and after surgery we find that the majority of patients are able to breath more healthily and thus are more energetic and fit, and this is very likely to continue throughout their life.
To have health in the universe is like being able to breath…